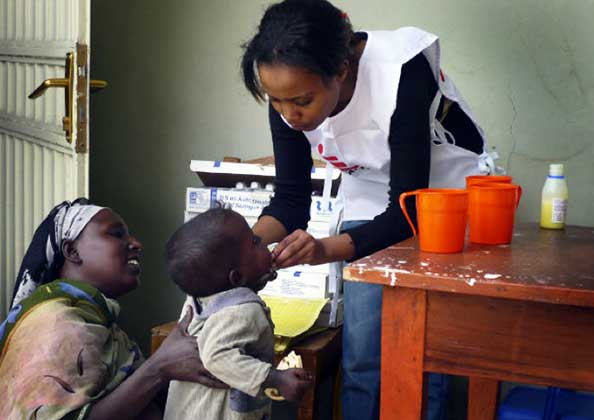
Dembe is a citizen of Uganda who resides in Tororo, a trading hub in the eastern region of Uganda that is 10 km from the border with Kenya. She works as a fishmonger in the local market and recently gave birth to a beautiful baby girl. As a mother of a newborn, she knows her daughter requires immunization but has yet to find a clinic that will offer this service. The most accessible health clinic to her in Uganda is unable to provide the needed vaccinations because of a stockout. In addition, the nurses at the clinic were unable to refer her to another clinic because they were not sure which one had an adequate supply of vaccines. Dembe considered visiting the next closest clinic, but it is located on the Kenyan side of Tororo, and she is not sure if the clinic would have the medicine her daughter needs. Furthermore, she has heard that the clinics in Kenya charge Ugandan citizens higher prices for immunization services because they aren’t citizens. Dembe faces a unique dilemma. She can’t risk any disruptions in her child’s healthcare and would benefit from easy access to healthcare services and referrals to clinics that could meet her needs.
Many cross-border town inhabitants, like Dembe, face similar issues of limited access to healthcare services. Cross-border communities are comprised of individuals that live along a nation’s borders. They are typically migrants and other mobile populations, such as pastoralists or those in the trucking industry, and may engage in economic activities or seek services on either side of the border. As the members of the communities interact with varied mobile populations, they are often at higher risk of vulnerabilities, such as infectious disease. This susceptibility makes it vital for them to have equitable access to healthcare services, on either side of the border, no matter what country they reside in.
Due to the above needs of migrants, global and regional organizations have developed policies to protect their rights. For instance, the Intergovernmental Authority on Development (IGAD) regional migration policy framework states that migrants must have access to healthcare services in order to protect them from disease and potential epidemics.
However, practices such as charging non-citizens more for services and discrimination based on disease status prevents some populations, such as those living in border towns, from accessing critical services. In addition, the lack of clearly defined policies and structures, that allow for tracking and follow-up of patients as
they progress back and forth between different countries’ health care systems, leads to inadequate quality data and unreliable medical records for cross-border populations. This results in compromised access to continued care for the patients. Furthermore, without sufficient data, country leadership is unable to properly plan and allocate resources for health care.
In an effort to address the issues stated above, the Regional Action through Data (RAD) initiative is working to promote the availability and use of data to drive performance in healthcare service delivery and thus improve health and development outcomes in Sub-Saharan Africa. Funded by USAID and led by Br
oadReach, RAD is composed of a consortium of members, including the Duke University Global Health Innovation Center (GHIC), IGAD, Jembi Health Systems, and the West African Health Organization (WAHO). The initiative aims to strengthen the capacity of member states to utilize existing data systems, promote collaboration across sectors, and improve the use of health data for decision-making.
In 2017, the Duke GHIC RAD team conducted a landscape policy analysis and participated in site visits along the border of Uganda and Kenya. The analysis revealed that while all IGAD member countries are investing in health data infrastructure, there are significant differences between countries in regards to data availability and use. While some countries stand out with significant progress and innovative practices in data sharing across the border, there are inconsistent patient confidentiality law
s across countries in the region. Additionally, there is no comprehensive law or legal framework for regional data sharing, data protection, or storage, thus limiting effective cross-border data sharing. This not only disrupts the continuity of care for cross-border and mobile populations, but also limits access and use of data by the governments themselves.
Furthermore, the team found that the lack of interlinked electronic medical record systems results in all patients acting as exchange mediums for their personal health records via handwritten patient reports. Although simple card and paper documents have the advantage of providing an integrated record of illness, attendances at facilities, and record of immunization for each person, their use as a critical component of record keeping has serious disadvantages, especially for mobile populations. This is because there is a high risk of paper records getting lost, destroyed, or becoming illegible, leading to loss of data.
RAD is developing multiple solutions to address the gaps noted in policy and practice. One consortium member, Jembi Health Systems, developed the Journey Solution, a platform that uses Near Field Communication (NFC) cards to allow individuals to carry their own electronic health data and permit easy access of their records by health professionals anywhere in the region. Through the RAD initiative, the Journey Solution is being piloted for immunization services in facilities in Kenya and Uganda.
In addition, Duke GHIC team is leading the development of a regional health data sharing and protection policy framework for IGAD member states. The policy framework, in line with best practices, will set out conditions for cross border health data transfer and aid IGAD member states to consider the appropriate safeguards to apply while sharing health data, thus maximizing the benefits of data-sharing while safeguarding the privacy and interests of individuals and the member states.
The regional data sharing policy and the digital Journey Solution seek to create an environment that will support people like Dembe and her family to make sure they have continuous access to quality health services, regardless of their country of origin or which facility they visit. In addition to the reduction of the risk of lost medical records of cross border mobile patients, countries will have access to treatment data allowing them to be able to forecast to ensure that there are enough drugs, human resources, and facilities to serve both their citizens and mobile populations.
The RAD initiative will ultimately create a conducive environment for health innovation and benefit cross-border and mobile populations by improving timely access to health services, improving continuity of care, and strengthening the use of data for decision making by leaders in the health sector.
Written by Nnennaya Asi & Juliana Hagembe
